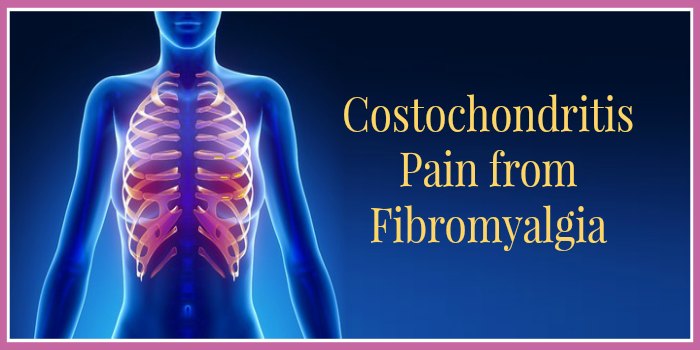
Costochondritis Pain from Fibromyalgia
 Costochondritis
CostochondritisCostochondritis pain is just one of the symptoms within Fibromyalgia. You have likely experienced it at one time or another.
This pain involves burning, stabbing, and radiating pain around the ribs and sometimes pushing up into the lower chest area.
It may not always occur as often as other symptoms such as widespread muscle pain
or nerve pain.
However, when it does occur, it can be very painful. If this is occurring more often for you, please get this checked out, as we don't want to miss another condition.
This pain can strike without warning and can be caused by a number of things like injury or trauma to the body and seems to occur more in people with fibromyalgia.
We also want you to be aware of other potential conditions that cause similar symptoms but might be something all together different.
Scary Symptoms
Imagine a busy mother of three young children. We’ll call her Terry. She’s buzzing through her evening routine, getting her little ones fed, bathed, and happily tucked into bed after a long story-reading session.
As one child brushes her teeth and another chatters endlessly from the bathtub, Terry sits on the edge of the tub. She leans forward, holding a hand over the left side of her chest.
She touches her ribcage, then the center of her chest, and she winces. She’s been tender in those areas for days, and now the severe pain has her bending over in agony.
In this situation, Terry might call 911, assuming that she’s having a heart attack. She would end up in the hospital going through a series of tests, and they would tell her that there is nothing wrong with her heart.
There’s nothing wrong with her at all. More than likely, she would return home with the same pain and a big question mark about the cause.
This type of unexplained chest pain is known as costochondritis. The cartilage connecting the ribcage to the breastbone becomes inflamed, leading to pain in the chest or ribcage. In some cases, the pain may extend to the arms and other surrounding areas.
While some people experience mild pain or annoying discomfort, others experience extreme pain that is sometimes mistaken as a heart attack. In some cases, the pain is so intense that the sufferer assumes that it has to be something serious.
Should You Worry About Costochondritis Pain?
 Chest Pain
Chest PainEven though as many as 70% of fibromyalgia sufferers experience chest pain at some point, this condition is not considered serious by medical professionals.
There is no risk to your life, and it won’t impact other areas of your body, as long as other conditions have been ruled out.
If you’re in severe pain or the condition lasts for a long period of time and interferes with your daily life, you may consider physical therapy or book an acupuncture session.
As long as more serious conditions have been ruled out by your doctor or another medical professional, managing the pain and discomfort is the best that you can do.
The Costochondritis-Fibromyalgia Connection
The onset of costochondritis pain can be related to car accidents, falls or other incidents that cause injury to the chest area.
It can sometimes develop if you have a severe upper respiratory infection as well.
Many people who don’t have fibromyalgia develop this painful condition due to injury or illness, but many with fibromyalgia also develop this painful and sometimes alarming symptom.
Remember that inflammation itself can also be caused by trigger points around the body.
Trigger points occur within layers of muscle and around connective tissue, so this area around the ribs can certainly become more vulnerable to radiating pain. A link to our trigger points article is located at the bottom of this article.
If you can trace the development of the pain back to an accident or an illness, then your fibromyalgia may intensify the pain.
The discomfort of costochondritis pain may also stimulate a flare-up of other fibromyalgia symptoms. We do believe that fibromyalgia itself can cause costochondritis pain without any other contributing factors.
What Should You Do When Chest Pain Hits?
It’s
important to seek medical attention right away if you experience pain
or discomfort in your chest. There are other conditions that could cause
this type of pain, including problems with your heart or gallbladder.
Once those more serious alternatives are ruled out, and you know that
there is no life-altering reason for your pain, you can treat the
discomfort through cold compresses or the breathing exercise I describe
in the last paragraph of this article. This will be similar to how you
may treat the symptoms of a fibromyalgia flare-up that are not
life-threatening.
Costochondritis can get worse when you cough,
take deep breaths, or move around. You may need to rest more and give
yourself a break until the pain subsides. If it becomes unmanageable,
seek medical attention to ask about alternative forms of treatment.
As a colon therapist, I would like to extend another caution, so as not
to miss other conditions. Another common condition that often mimics
the pain of costochondritis is liver or bile duct pain. You could be
having gallbladder attacks and not know it. If you are having pain
around the upper front of the rib cage, along the transverse colon area
(same area), you need to be aware of this potential issue and rule that
out as well.
If you are experiencing costochondritis symptoms
and are having difficulty breathing because of the pain/spasms around
the chest and ribs, try this simple technique. Sit comfortably in a
chair, with feet on floor. Take your hands crossed on your chest, and
them move yourself forward from the waist, leaning over while sitting
and see if that allows you to obtain some better breathing.
You see, the inability to breathe properly during this kind of episode can actually make this pain intensify. So the best thing you can do, is to find a comfortable position in which you can better breathe and not hold the tension so much in these areas.
Be aware of side sleeping.
I find that for myself, if I am sleeping on my side for a long period of time during the night, this has the potential to bring on costochondritis pains.
What about compression?
Remember how I often talk about using light to moderate compression on certain areas of the body to increase blood flow? Hands, feet, knees, etc. Well, we can also use light compression around the ribs. If store bought abdominal wraps are too tight or uncomfortable for you, experiment by cutting up smaller pieces of clothing like shirts, and then using them for compression.
We also find there can be a correlation between trigger points and costochondritis. This can occur from any kind of injury, strain, surgery, etc.
You can read more here at Trigger Points and Fibromyalgia.
Below you will see one of my favorite remedies for inflammation. Astazanthin can help our bodies in more ways than one, and I like to include this in our toolbox of remedies for treating inflammation.
Before you leave, my sitemap can provide you with a "God's-eye" view of this website laid out in "outline format".
Stay connected by using the contact form below.
Home > Fibromyalgia Symptoms > Costochondritis Pain from Fibromyalgia
Didn't find what you were looking for? Search for it:
living-smarter-with-fibromyalgia.com
©2013-2025 All Rights Reserved
FibroFitPeople, LLC ;©2025 All Rights Reserved